The fundamental difference between palliative care and hospice really comes down to two things: timing and the goals of treatment.
Palliative care is an extra layer of support that can start the moment someone is diagnosed with a serious illness. The key here is that it’s provided alongside curative treatments—like chemotherapy or surgery—to manage symptoms and improve quality of life. Think of it as comfort-focused care that complements the primary medical plan.
On the other hand, hospice care is reserved for individuals with a life expectancy of six months or less who are no longer pursuing treatments to cure their illness. At this stage, the entire focus shifts to providing comfort, peace, and dignity.
A Foundational Look at Two Care Philosophies

Making sense of palliative care vs. hospice is crucial when navigating a difficult health journey. While both are rooted in compassion and support, they are designed for different needs at different times.
Hospice is actually a specific type of palliative care, but it’s tailored for the final phase of life. This distinction is more than just semantics; it directly impacts everything from the medical services provided to what insurance will cover. Grasping this helps families make the most informed choices.
Key Differences Between Palliative Care and Hospice at a Glance
To make this even clearer, let's break down the core distinctions in a simple table. This gives you a quick snapshot of where these two approaches diverge, which can be a great starting point for conversations with doctors and family members.
| Feature | Palliative Care | Hospice Care |
|---|---|---|
| Primary Goal | Relieve symptoms and improve quality of life while undergoing treatment. | Provide comfort, compassion, and dignity at the end of life. |
| When It Begins | At any stage of a serious illness, often at diagnosis. | When life expectancy is six months or less and curative treatment stops. |
| Treatment Focus | Can be provided alongside curative treatments like chemotherapy. | Focuses exclusively on comfort care; curative treatments are discontinued. |
| Typical Location | Hospitals, outpatient clinics, long-term care facilities, and at home. | Primarily in the patient's home, but also in dedicated hospice facilities. |
As you can see, these two options represent different philosophies of care designed for specific stages of an illness. While they both aim to provide comfort, their eligibility and application are what truly set them apart. It's also helpful to understand how these services are delivered in the home, which is why we've put together a detailed guide explaining the differences between home health and home care.
Understanding Palliative Care: An Extra Layer of Support

There’s a common misconception that palliative care is only for the very end of life. That’s just not true. It’s actually a crucial, extra layer of support available to anyone with a serious illness, right from the moment of diagnosis. The whole point is to improve quality of life for both the patient and their family.
This specialized medical care is all about providing relief from the symptoms and stress that come with a serious illness. The goal is to manage discomfort, make communication clearer, and ensure the treatment plan truly aligns with a person’s own values and goals. It’s about treating the whole person, not just the disease.
This means a dedicated team steps in to manage physical symptoms like pain, nausea, and fatigue. At the same time, they offer vital emotional, social, and spiritual support, helping patients and their loved ones navigate the challenges that a difficult diagnosis brings.
Palliative Care Works with Curative Treatment
One of the most important things to understand in the palliative care vs. hospice discussion is that palliative care can be provided alongside curative treatments. Someone can absolutely receive palliative services while actively undergoing chemotherapy, radiation, or even while preparing for surgery.
Palliative care is about living as well as possible, for as long as possible. It helps patients gain the strength to carry on with their daily life and tolerate medical treatments.
Think about someone diagnosed with a chronic respiratory disease. While they continue their primary treatments to manage the illness, a palliative team can help them control breathing difficulties, manage anxiety, and maintain their independence at home. It’s a collaborative approach that makes comfort a priority throughout their entire health journey.
The need for this kind of support is massive. The World Health Organization estimates that globally, millions require palliative care, often for conditions like cardiovascular diseases (38%), cancer (34%), and chronic respiratory diseases (10.3%). You can dive deeper into the data on global palliative care needs by reading these important findings on the Annals of Palliative Medicine website.
A Team-Based Approach to Comfort
The real strength of palliative care is its multidisciplinary team, which is a group of specialists working together for you. This team often includes:
- Palliative Care Doctors and Nurses: Experts who specialize in managing pain and other difficult symptoms.
- Social Workers: Professionals who can help with the practical stuff, like navigating insurance or finding community resources.
- Chaplains or Spiritual Advisors: Individuals who offer spiritual support that’s tailored to the patient’s personal beliefs.
- Therapists: Specialists who can provide counseling for emotional distress or help with physical rehabilitation.
This team works in partnership with you, your family, and your other doctors to create a truly integrated system of support. By addressing such a wide range of needs, palliative care helps ensure the focus always stays on the patient’s overall well-being.
Defining Hospice Care: Comfort and Dignity for Life's Final Chapter
When a serious illness gets to an advanced stage, the entire focus of care naturally shifts. This is where hospice care comes in, offering a special kind of support that’s all about comfort, dignity, and finding peace during the final phase of life. It’s a very different path from palliative care, because hospice isn't provided alongside treatments meant to cure an illness.
Instead, hospice begins when a patient, their family, and their doctor all agree to stop curative treatments. That decision signals a new set of goals—moving away from fighting the disease to making the most of the quality of life for whatever time remains. The whole idea behind hospice is to make sure a person's last months are lived with as little pain as possible, ideally surrounded by the people they love.
Strict Eligibility for Specialized Comfort
To qualify for hospice, you have to meet specific criteria, which really sets it apart from the much broader field of palliative care. A doctor must certify that the patient has a terminal illness and, if the disease runs its natural course, is expected to live for six months or less.
This clear timeline is a fundamental difference when you're looking at palliative care vs. hospice. It ensures hospice resources are focused on those who truly need this unique, end-of-life support. Once a person is enrolled, their care plan is completely built around managing symptoms and providing deep emotional and spiritual support.
Hospice care affirms life and regards dying as a normal process. It neither hastens nor postpones death but exists to provide comfort and support for patients and their families when a cure is no longer possible.
A Holistic Approach for Patient and Family
Hospice care is so much more than just managing medical issues; it’s a full-circle support system for the entire family. The care team looks at a wide spectrum of needs to make sure both the patient and their loved ones feel supported through what is an incredibly difficult journey.
This team-based approach almost always includes:
- Pain and Symptom Management: Using expert medical care to get pain, shortness of breath, and other difficult symptoms under control.
- Emotional and Spiritual Counseling: Offering support for patients to work through feelings of anxiety, depression, or to address spiritual questions.
- Family Support and Education: Guiding family members on how to best care for their loved one and helping them know what to expect.
- Bereavement Services: Providing counseling and support groups for the family for up to a year after their loved one has passed away.
Think about a family dealing with the final stages of congestive heart failure. A hospice team could manage the patient's physical discomfort right at home, while a social worker helps the family cope with the emotional stress and a spiritual counselor provides a sense of peace. This complete approach is the hallmark of quality in-home hospice care because it supports everyone involved, making a real difference during a deeply personal time.
A Side-by-Side Comparison of Services and Goals
Knowing the philosophical differences between palliative care and hospice is a great start. But now, let's get into the practical details that families really need to know. A direct comparison helps cut through the confusion and shows you what palliative care versus hospice looks like in the real world, making it easier to see which path fits your family's needs.
We'll look at who qualifies, what the goals of treatment are, where care happens, and how it’s all paid for. Each of these areas reveals a key difference that can heavily influence your decision.
Eligibility and Timing of Care
The single biggest difference comes down to when each type of care can begin. Palliative care is available at any stage of a serious illness, often starting right from the day of diagnosis. There’s no requirement for a specific life expectancy, which makes it an incredibly flexible support system for anyone navigating the symptoms and stress of a chronic condition.
Hospice care, on the other hand, has a much clearer entry point. A person only becomes eligible for hospice when two doctors certify that they likely have a life expectancy of six months or less if the illness progresses naturally. This prognosis is precisely why hospice is considered end-of-life care.
Core Treatment Philosophy and Goals
This is where you can really see the intent behind the care diverge. The main goal of palliative care is to improve quality of life while a patient continues to receive curative treatments. The palliative team works right alongside a patient’s other doctors to manage pain and other symptoms, but the overall medical plan might still be aimed at curing the disease.
Hospice care starts when the focus shifts entirely away from a cure and toward comfort. All medical care and support services are geared toward symptom relief, peace, and dignity. Curative treatments, like chemotherapy or radiation, are stopped because they no longer align with the patient’s goals for their remaining time.
The core difference is simple: Palliative care is "comfort care with curative treatment," while hospice is "comfort care instead of curative treatment." Understanding this distinction is vital for making an informed choice.
This visual helps break down the key differences in eligibility, care settings, and insurance coverage.
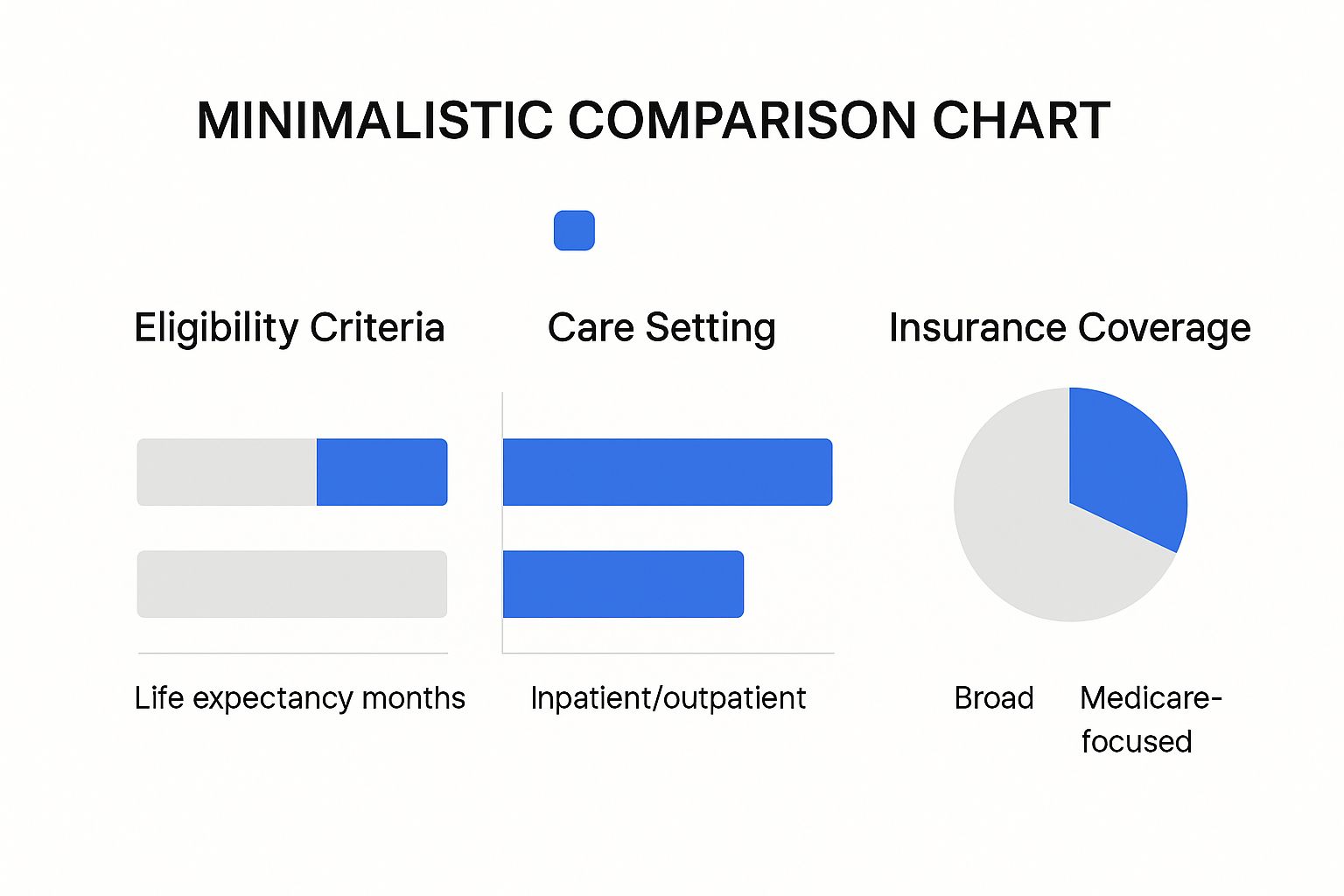
As the chart shows, the flexibility of palliative care in its timing and treatment approach stands in sharp contrast to the specific, end-of-life focus of hospice.
Scope of Services and Care Settings
Both palliative and hospice care rely on an interdisciplinary team, but the environment and the scope of services can look quite different.
- Palliative Care: You’ll often find these services delivered in hospitals, outpatient clinics, or long-term care facilities. While home-based palliative care is becoming more common, it often starts in a clinical setting.
- Hospice Care: This care is primarily provided wherever the patient calls home. That could be a private house, an assisted living community, or a nursing home. The whole point is to allow the person to stay in a familiar, comfortable place.
While they serve related purposes, the availability of palliative and hospice care varies significantly around the world. As of 2017, an estimated 7 million patients globally received some type of palliative care. To put that in perspective, hospice care—a specific type of palliative care—was provided to about 1.49 million beneficiaries in the U.S. alone, supported by 4,515 certified providers. You can find more details on the global utilization of these care types.
To help clarify these distinctions, here's a detailed breakdown of the features side-by-side.
Palliative Care vs Hospice Detailed Feature Breakdown
| Aspect | Palliative Care | Hospice Care |
|---|---|---|
| Eligibility | Any stage of a serious illness, no prognosis needed. | Terminal illness diagnosis with a life expectancy of 6 months or less. |
| Treatment Goals | Relieve symptoms and stress while pursuing curative treatments. | Focus on comfort, quality of life, and dignity. Curative treatments are stopped. |
| Typical Duration | Can be provided for years, depending on the illness. | Limited to the final months of life. |
| Care Team | Doctors, nurses, social workers, and other specialists. | Same as palliative, but also includes chaplains, volunteers, and bereavement counselors. |
| Care Setting | Hospitals, outpatient clinics, long-term care, some home settings. | Primarily at home, but also in assisted living, nursing homes, or hospice facilities. |
| Insurance Coverage | Covered by Medicare Part B, Medicaid, and private insurance. | Primarily covered by the Medicare Hospice Benefit and most private insurance. |
This table makes it easy to see how the two models are structured to meet very different needs at different points in a person's health journey.
How Care Is Paid For
Finally, let’s talk about the financial side of the palliative care vs. hospice discussion. Palliative care is usually covered by private insurance, Medicare Part B, and Medicaid, much like any other specialist medical service. Depending on their plan, patients might have co-pays or deductibles to meet.
Hospice care is a different story. It is most often covered entirely by the Medicare Hospice Benefit. This is an all-inclusive benefit that covers nearly everything related to the terminal illness—including medications, medical equipment, and the services of the hospice team—with little to no out-of-pocket costs for the patient.
How to Choose Between Palliative and Hospice Care

Trying to decide between palliative care and hospice can feel like an impossible task, but it gets much simpler when you anchor the decision in the patient's immediate goals and medical reality. The right path forward depends entirely on the specific situation, and looking at a few real-world examples can make the choice much clearer.
This isn't just a medical decision; it's a deeply personal one. It involves balancing the potential benefits of aggressive, curative treatments against the desire for comfort, peace, and quality of life. Walking through these scenarios can give you a practical framework for what is often a very difficult conversation.
When to Choose Palliative Care
Palliative care is the right call when the main objective is to relieve symptoms and boost quality of life while still actively pursuing curative treatments. Think of it as an extra layer of support, not a substitute for the patient's primary medical team.
Here's a common situation:
- Scenario 1: A patient newly diagnosed with multiple sclerosis. They're dealing with serious pain, fatigue, and muscle spasms that get in the way of their daily life. At the same time, they are working closely with their neurologist on a long-term plan to slow the disease's progression. Palliative care is a perfect fit here. A dedicated team can zero in on managing these tough symptoms, which helps the patient better tolerate their primary treatments and hang on to their independence.
The question that defines palliative care is this: "How can we make life better right now, even as we continue fighting the underlying illness?" It's all about living better with a serious diagnosis.
When to Choose Hospice Care
Hospice becomes the appropriate choice when the focus pivots away from curing the illness and toward maximizing comfort for the time that’s left. This usually happens when treatments are no longer working or when a patient decides that the side effects and burdens of treatment are greater than the potential benefits.
Let's look at another example:
- Scenario 2: An individual with end-stage kidney disease. After years of dialysis, the treatments have become exhausting and are causing severe side effects that are crushing their quality of life. After many conversations with their doctor and family, they decide to stop dialysis. This is the point where a transition to hospice makes sense. The hospice team will step in to manage symptoms like pain and shortness of breath, provide crucial emotional and spiritual support, and make sure the patient can live their final months at home with peace and dignity.
Starting the Conversation
Bringing up palliative or hospice care takes a lot of courage and sensitivity. It’s usually best to approach the conversation by focusing on the patient's own wishes and goals. Rather than dwelling on the terminal aspect of an illness, open the door by asking what's most important to them.
Here are a few gentle ways to start:
- "What are you most worried or fearful about with your health right now?"
- "If there was one thing we could fix about your day-to-day life, what would it be?"
- "Have you given any thought to the kind of care you'd want if your condition changes?"
Talking about care options will almost certainly bring up financial concerns. Understanding how different types of care are covered is critical, as the costs can be a major source of stress. To help you prepare, it's a good idea to get familiar with how major insurance programs work by reviewing our guide on Medicare vs. Medicaid coverage.
Ultimately, this is a shared decision between the patient, their family, and their medical providers. While the choice is a big one, remember that both palliative and hospice care share the same mission: to provide compassionate, person-centered support. The need for these services is huge, yet global access is surprisingly limited. In fact, only 15% of countries offer high-level palliative care, and the U.S. ranks 43rd out of 81 countries in the quality of its end-of-life care, despite high healthcare spending. You can read more on these global gaps in this detailed report. This just underscores how important it is to advocate for the right care at the right time.
Common Questions About Palliative and Hospice Care
When you're exploring the differences between palliative care and hospice, a lot of practical questions naturally come up. Getting straight answers is the first step toward making a confident decision and making sure your loved one gets the right kind of support for their needs.
Let's clear up some of the most common uncertainties families run into.
Can a Patient Receive Both Palliative Care and Hospice?
This is a really common point of confusion, but the answer is surprisingly straightforward: no. You can't be enrolled in a standard palliative care program and the Medicare hospice benefit at the same time.
Think of it this way: hospice is actually a very specialized type of palliative care. When someone chooses to receive hospice care, that team becomes the main source of support for their terminal illness. They take over managing symptoms and ensuring comfort, which means a separate palliative care team is no longer needed. The decision to start hospice marks a shift in goals—moving away from curative treatments and toward comfort-focused care.
What if Someone on Hospice Lives Longer Than Six Months?
A doctor's prognosis is an educated guess, not a hard deadline. It’s actually not unusual for someone on hospice to live longer than the initial six-month projection. If this happens, it doesn’t mean they’ll automatically be disqualified from care.
Instead, a patient's eligibility is simply reviewed from time to time. As long as their physician and the hospice medical director recertify that their prognosis is still six months or less, they can continue receiving hospice services. In some wonderful cases, a person's condition might stabilize or even get better. When that happens, they can be discharged from hospice and are free to go back to curative treatments if they wish.
The real goal of hospice is to give someone the best possible quality of life for whatever time they have left, whether that's days, weeks, or many months. The focus is always on the patient's immediate needs, not a calendar.
How Do We Start the Conversation About This Type of Care?
Bringing up palliative or hospice care is a delicate conversation, and it needs to be handled with a lot of sensitivity. The trick is to frame it as a way to improve quality of life, not as a sign of giving up. Keep the focus on the benefits—like adding another layer of support to help manage tough symptoms and take some of the stress off everyone.
Here are a few ways to gently start that important discussion:
- Focus on Quality of Life: Start by talking about what they're going through right now. You could say something like, "I've noticed you've been in a lot of pain lately. There's a type of care that's all about managing symptoms like that, and it could help you feel so much better."
- Frame it as Added Support: Present it as a way to boost their current medical plan, not replace it. For example, "What if we brought in a team of experts whose only job is to focus on making you comfortable?"
- Suggest an Informational Meeting: Propose a no-pressure consultation. Suggesting a chat with a palliative or hospice specialist just to learn about the options can feel a lot less scary than making a final decision on the spot.
This conversation is the first step toward making sure the care plan truly lines up with what matters most to your loved one.
At NJ Caregiving, we know how challenging these conversations can be. Our compassionate team is here to give your family the support and guidance you need to get through these decisions with confidence. To learn how our in-home care services can improve your loved one's comfort and quality of life, visit us at https://njcaregiving.com.


