Yes, Medicare absolutely helps pay for home health care. But here's the catch every family needs to understand: it’s only for medically necessary, skilled services that are short-term and intermittent.
This is a really important point. Medicare isn't designed to cover long-term custodial support, like someone helping with meal prep or bathing every day. Think of it as medical care that comes to you when you need it, not as a round-the-clock caregiver.
Your Quick Answer on Medicare Home Health Coverage
When a doctor says your loved one needs care at home after a hospital stay or to manage an illness, one of the first questions is always, "How are we going to pay for this?" For millions of families, Medicare is a huge part of the answer. Figuring out what it covers is the first step toward getting the right support.

What Does Medicare Home Health Actually Mean?
The key is to draw a line between medical care and personal assistance. Medicare’s benefit is like having a visiting nurse or a physical therapist come to your home to help you recover—not someone who helps with daily chores indefinitely.
This benefit is a cornerstone of senior healthcare in America. In fact, Medicare is the single largest payer for home health services in the country, covering about 42% of all home health visits. This makes it a lifeline for countless seniors trying to recover and age comfortably right where they want to be: in their own homes. You can review more home health statistics to see the full picture of its impact.
So, let's break it down to make it simple.
Medicare Home Health Coverage At a Glance
To help families in Princeton, Hamilton, and across Mercer County see where the lines are drawn, here’s a quick summary of what Medicare Part A and Part B typically cover versus what they don’t for home health care.
| Category | What Medicare Typically Covers | What Medicare Typically Does NOT Cover |
|---|---|---|
| Nursing Services | Part-time skilled nursing care | 24/7 in-home care |
| Therapy Services | Physical, occupational, and speech therapy | Homemaker services like shopping or cleaning |
| Personal Care | Home health aide services (only if you also need skilled care) | Custodial care (bathing, dressing) if it’s the only care you need |
| Supplies & Equipment | Medical supplies for your care and durable medical equipment (with 20% coinsurance) | Meal delivery services or prescription drugs |
This table gives you a starting point. As you can see, Medicare is focused on the "health" part of home health care, stepping in when there's a specific medical need and a plan for recovery or management. It leaves the day-to-day, non-medical support to other resources.
What Medicare Considers Home Health Care
When you hear the term “home health care,” it’s easy to picture someone helping with daily chores and offering companionship. But when it comes to Medicare, that's not quite what they mean.
Medicare’s definition is very specific. It refers to a distinct set of skilled, medical services a doctor orders to help you recover from an illness or injury, or to manage a serious health condition right from your own home.
Think of it less like a helper and more like a clinical team that comes to you. Their mission isn't to handle everyday household tasks indefinitely. Instead, they arrive with a clear, doctor-prescribed plan to provide targeted medical care and therapy. The goal is always to help you get back on your feet, regain your independence, and improve your health.
This type of care is always part-time or intermittent, meaning it’s delivered through scheduled visits—not 24/7. It’s a goal-oriented process with a clear finish line in sight.
The Core Skilled Services Covered
For Medicare to step in, a doctor must certify that you need at least one of four specific types of skilled care. These services form the backbone of the Medicare home health benefit.
-
Skilled Nursing Care: This is the most common requirement. Provided by a Registered Nurse (RN) or Licensed Practical Nurse (LPN), it covers clinical tasks like changing wound dressings, giving IV drugs or injections, and teaching you or your family how to manage a new medication or health condition.
-
Physical Therapy (PT): After a fall, surgery, or illness, a physical therapist can be a game-changer. They work with you to restore movement, build strength, improve balance, and manage pain, helping you walk and move safely again.
-
Occupational Therapy (OT): Occupational therapists are experts in the "occupations" of daily living. If a stroke has made getting dressed or preparing a meal difficult, an OT can teach you new, safe ways to perform these essential activities and regain your day-to-day function.
-
Speech-Language Pathology Services: Also known as speech therapy, these services are for more than just talking. A speech pathologist helps with communication issues after a stroke, but they also work with patients who have trouble swallowing, helping them learn to eat and drink safely.
The bottom line is that Medicare home health care is fundamentally restorative or maintenance-based. It’s designed to either help you get better and back to your old self, or to maintain your current condition and stop it from getting worse.
What About Help with Daily Activities?
This is where a lot of families run into confusion. What about essential help with things like bathing, getting dressed, or using the bathroom? These tasks are known as home health aide services.
Here’s the crucial part: Medicare will pay for a home health aide, but only under one condition. You must also be receiving skilled care, like nursing or therapy, at the same time. The aide’s job is seen as support for the primary medical care you’re getting.
So, if a nurse comes to your home three times a week to care for a surgical wound, Medicare might also approve a home health aide to help you bathe on those days. But if you only need help with bathing and don't have a qualifying need for skilled care, Medicare won’t cover it. That skilled medical need is the anchor that all other covered services depend on.
Meeting the Four Pillars of Eligibility
Figuring out if Medicare will pay for home health care can feel confusing, but it really boils down to meeting four specific requirements. I like to think of these as the four legs of a table—if you take one away, the whole thing gets wobbly. Getting these four things right is the difference between having that vital in-home medical support covered and facing a frustrating denial.
For families here in Mercer County and for hospital discharge planners, understanding these pillars takes the guesswork out of the equation. It gives you a clear checklist to see if your loved one actually qualifies for this benefit.
Pillar 1: Your Doctor Must Be in Charge
First off, everything starts with your doctor. You have to be under their active care, and they need to set up a formal plan of care. This isn't just a casual suggestion; it's a documented plan that your physician creates, reviews regularly, and officially certifies.
Think of this plan as the official roadmap for all the home health services. It spells out exactly what medical care is needed, which types of services will be provided, how often the visits will happen, and what the goals of the treatment are. Your doctor is the one driving this process from start to finish.
Pillar 2: You Need Certified Skilled Care
The second pillar is probably the most critical: you must have a medical need for skilled services. Your doctor has to certify that you require intermittent skilled nursing, physical therapy, speech-language pathology, or ongoing occupational therapy. This is the real key to eligibility.
Needing a hand with daily activities like bathing, getting dressed, or making meals isn't enough on its own. It's the need for a licensed, skilled professional that unlocks the entire Medicare home health benefit.
This visual helps break down the difference between the medical care Medicare covers and the personal assistance it generally doesn't.
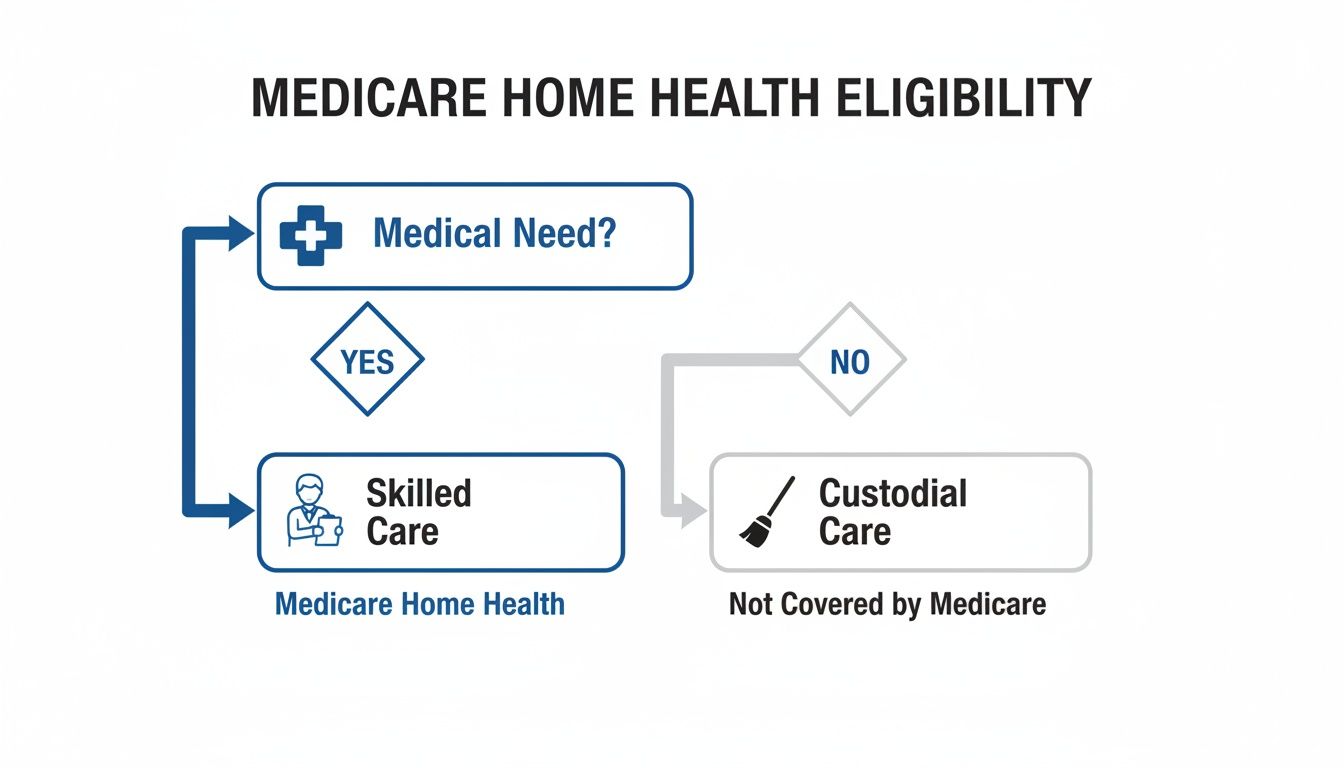
As the chart shows, the path to getting Medicare coverage always starts with a documented medical issue that requires a skilled professional, not just general support.
Pillar 3: You Must Be Certified as Homebound
Next, a doctor needs to certify that you are homebound. This term trips a lot of people up. It absolutely does not mean you're confined to your bed or can never, ever leave the house.
Medicare considers you homebound if leaving your home requires a considerable and taxing effort. This might be because of an illness or injury where you need help from another person or special transportation to get out. You can still leave for medical appointments, and even short, infrequent trips for non-medical reasons (like going to a religious service) are usually okay.
This rule is just to make sure the benefit goes to people who can't easily get to a clinic or doctor's office for their care. If you want to dig a little deeper into the specifics, our guide on Medicare home health requirements provides a lot more detail.
Pillar 4: Use a Medicare-Certified Agency
Finally, the care has to come from a home health agency that is officially certified by Medicare. These agencies have passed federal inspections for patient safety and quality of care. If you use an agency that isn't certified, Medicare won't pay a dime, even if you meet all the other criteria perfectly.
Nailing down these four pillars is non-negotiable. By working with your medical team to confirm each one, you can move forward with confidence, knowing that Medicare will be there to help your loved one recover safely in the comfort of their own home.
Understanding Your Costs and Coverage Limits
It's the question on every family's mind: what is this going to cost? The good news is that when it comes to approved home health care, Medicare often covers 100% of the cost. For the core services—skilled nursing and various therapies—there are typically no deductibles or copayments under Original Medicare. That can be a huge weight off your shoulders during an already stressful time.
But it’s important to know that this coverage isn't a blank check for unlimited care. Medicare is very specific about how long and how often it will pay for these services. Getting a handle on these limits will help you set realistic expectations for your loved one's care.
The "Part-Time and Intermittent" Rule
Medicare funds home health care that it defines as "part-time or intermittent." This is the key phrase to remember. The benefit is designed for recovery and stabilization, not for round-the-clock or long-term daily support.
While there's some flexibility, this generally breaks down to:
- A combined total of up to 28 hours per week for skilled nursing and home health aide services.
- In some less common situations, this can be bumped up to 35 hours per week, but only if a doctor provides very clear documentation explaining why it's medically necessary.
The care also needs to be predictable and finite. Your doctor is required to review and recertify the entire plan of care every 60 days, confirming that the services are still essential for your loved one's condition.
Think of it like a prescription for physical therapy. A doctor orders a specific number of sessions to help you reach a goal, like regaining strength after surgery. Medicare home health is prescribed in the same way—in 60-day episodes—with the goal of getting better or stable, not providing indefinite support.
Paying for Durable Medical Equipment
While the skilled care services are covered at 100%, there is one area where you’ll likely have an out-of-pocket cost. If the care plan calls for durable medical equipment (DME)—things like a walker, a hospital bed, or oxygen equipment—you’ll be responsible for part of the bill.
After you've met your annual Part B deductible, you will pay 20% of the Medicare-approved amount for any necessary DME. This coinsurance is an important detail to factor into your financial planning as you set up care at home.
Figuring out these potential costs is a key piece of the puzzle. For a bigger picture of your financing options, take a look at our guide on how to pay for home care. By understanding both what Medicare covers and where the limits are, you can build a much more complete and sustainable care plan for your family.
Medicare, Medicaid, and Advantage Plans: What’s the Difference?
Trying to figure out home health coverage can feel like learning three different languages at once. You've got Original Medicare, Medicare Advantage, and Medicaid, and each one plays by its own set of rules. Understanding how they differ is the key to making the right choice for your family.
Think of Original Medicare as the baseline—a federal program with a standard set of rules that apply to everyone, no matter where you live. It pays directly for skilled home health care, but only if you meet its very specific medical criteria.
Medicare Advantage and Medicaid, however, work quite differently.
The Medicare Advantage Approach
If your loved one has a Medicare Advantage (Part C) plan, don't worry—they still have a right to home health care. These plans are legally required to cover everything that Original Medicare covers, including part-time skilled nursing, physical therapy, and other critical medical services at home.
But here’s the catch: the how is different. Medicare Advantage plans are run by private insurance companies, which means they operate with specific provider networks. You absolutely must use a home health agency that is in-network with your specific plan to get full coverage. Step outside that network, and you could be facing huge out-of-pocket bills or even a total denial of coverage.
Another hurdle is prior authorization. Most Advantage plans require the insurance company to approve the care as medically necessary before services can start. This is an extra step that can sometimes cause frustrating delays when care is needed right away.
The Critical Role of New Jersey Medicaid
Medicaid is a completely separate program from Medicare. While Medicare is based on your age or a disability, Medicaid is designed to help people with limited income and resources. This distinction becomes incredibly important when you start talking about long-term care.
The single biggest difference is that Medicare does not pay for long-term custodial care—the ongoing, non-medical help with daily activities like bathing, dressing, and meal preparation. Medicaid, however, often does.
Here in New Jersey, the Managed Long Term Services and Supports (MLTSS) program is built specifically to provide this kind of help. For those who qualify financially, NJ Medicaid can cover the exact type of personal care that Medicare won't touch. This is what allows many seniors to remain safely in their own homes for the long haul.
We have a complete guide that breaks this down even further. You can learn more about the differences between Medicare vs. Medicaid coverage to get a clearer picture.
Home Health Coverage: Original Medicare vs. Medicare Advantage vs. Medicaid
Seeing the programs side-by-side really helps clarify their different roles. Each is designed for a specific purpose, and knowing which one fits your needs is the first step toward building a sustainable care plan.
| Feature | Original Medicare (A & B) | Medicare Advantage (Part C) | New Jersey Medicaid (MLTSS) |
|---|---|---|---|
| Primary Goal | Short-term, skilled medical recovery after an illness or injury. | All-in-one health coverage that bundles Medicare benefits, managed by a private insurer with network rules. | Long-term health and personal care support for individuals with financial need. |
| Key Covered Services | Skilled nursing, Physical Therapy (PT), Occupational Therapy (OT), Speech-Language Pathology (SLP). Strictly medical. | Same skilled care as Original Medicare, but may include extra benefits like dental or vision. | Long-term custodial care (bathing, dressing, meal prep, toileting), plus skilled nursing if needed. |
| Provider Choice | Freedom to choose any Medicare-certified home health agency. | Must use a home health agency that is in-network with the specific plan. | Must use a home health provider that is approved by and contracted with New Jersey Medicaid. |
| Main Qualifier | A doctor certifies a medical need, and the patient must be considered "homebound." | Medical need is still required, but the plan's prior authorization and network rules are the main gatekeepers. | Based on financial need (strict income and asset limits must be met). |
It's also worth remembering that other financial supports exist beyond these major programs. It can be helpful to explore various healthcare grant opportunities that may assist with costs that insurance doesn't cover.
Ultimately, each program serves a unique purpose. The key is to match your loved one's specific health needs—and financial situation—to the right resource.
Your Next Steps for Getting Care in New Jersey
Knowing the rules is one thing, but taking action is what really brings your family peace of mind. If you're here in New Jersey and trying to figure out what to do next, working with a local, Medicare-certified agency like NJ Caregiving can make the whole process much smoother. Think of us as your guide—we’re here to translate the confusing requirements into a simple, clear plan.
It all starts with a conversation. We’ll sit down with you to get a real sense of your loved one's needs and answer all your questions about how Medicare covers home health care. From there, we work hand-in-hand with their doctor to get the official plan of care established and certified, which is a must-have for Medicare.

Building a Complete Care Solution
One of the biggest hurdles families run into is that Medicare pays for skilled medical needs, but not for personal care—things like help with bathing or getting dressed. This is where an experienced local agency can truly bridge the gap. We build a complete support system by combining Medicare-covered services with private-pay options for that essential personal assistance.
Here’s a quick look at how that unified approach works in practice:
- Medicare-Covered Care: We bring in the skilled nursing and therapy services that the doctor has ordered and Medicare will pay for.
- Private-Pay Personal Care: At the same time, we can provide compassionate aides to help with daily activities like bathing, dressing, and preparing meals.
This integrated model means every need is met, all under one roof. You aren’t left trying to coordinate multiple agencies.
You don't have to navigate this alone. A dedicated local partner handles the Medicare paperwork, coordinates with doctors, and creates a single care plan that covers both skilled health and personal support, ensuring your loved one receives complete, dignified care at home.
By taking care of the logistics and blending these different types of care, we free you up to focus on what’s most important—your family’s well-being.
Common Questions We Hear About Medicare Home Care
When you're trying to figure out Medicare's home health benefits, a lot of specific, practical questions come up. Getting straight answers is the first step to understanding what this important benefit can and can't do for your family.
Let's walk through some of the questions we hear most often.
Does Medicare Cover 24-Hour Care at Home?
This is a big one, and a frequent misconception. The short answer is no. Original Medicare is specifically designed to cover intermittent or part-time skilled care only. It simply wasn't built to pay for round-the-clock assistance.
For that kind of continuous, 24-hour care, families usually need to look at private pay options or see if their loved one qualifies for certain state-based Medicaid waiver programs.
What if Someone Isn’t Technically Homebound?
This is non-negotiable. To qualify for this particular Medicare benefit, a doctor must certify that the patient is homebound. It's a strict requirement. If a person can leave their home without it being a major, difficult effort or without the help of another person, they won't meet this key rule.
In those cases, they would likely need to explore getting therapy at an outpatient facility instead of having a professional come into the home.
Can We Get Medicare to Pay for Help with Just Bathing and Meals?
No, Medicare won't pay for what it calls "custodial care"—things like help with bathing, getting dressed, or making meals—if that's the only kind of help a person needs.
These personal care services, while essential, are only covered if they are part of a larger, skilled-care plan. They have to be necessary to support the main medical treatment, not the other way around. For standalone personal care, you'll need to find other resources.
While you're focused on care coverage, it's also a good time to think about legal healthcare documents. Many families find it helpful to learn the differences between a Living Will and Power of Attorney to make sure all their bases are covered.


