The Neuroscience of Communication in Dementia
Communicating with someone experiencing dementia can sometimes feel like trying to understand a different language. Our usual ways of talking don't always work, which can be frustrating for both the person with dementia and their caregiver. This communication breakdown happens because of key changes in the brain's communication hubs. Dementia disrupts the neural pathways that control how we process language, recall memories, and understand what we hear and see. This means familiar words, phrases, and even the faces of loved ones can become difficult to recognize or understand.
How Dementia Impacts Language and Memory
These neurological shifts show up in a variety of ways. For instance, someone with dementia might struggle to find the right word (anomia), have trouble following group conversations, or find it difficult to grasp abstract ideas. Short-term memory loss is also common, leading to repeated questions or forgetting recent events. Furthermore, dementia can affect executive functions, which makes it harder to plan, organize thoughts, and start conversations.
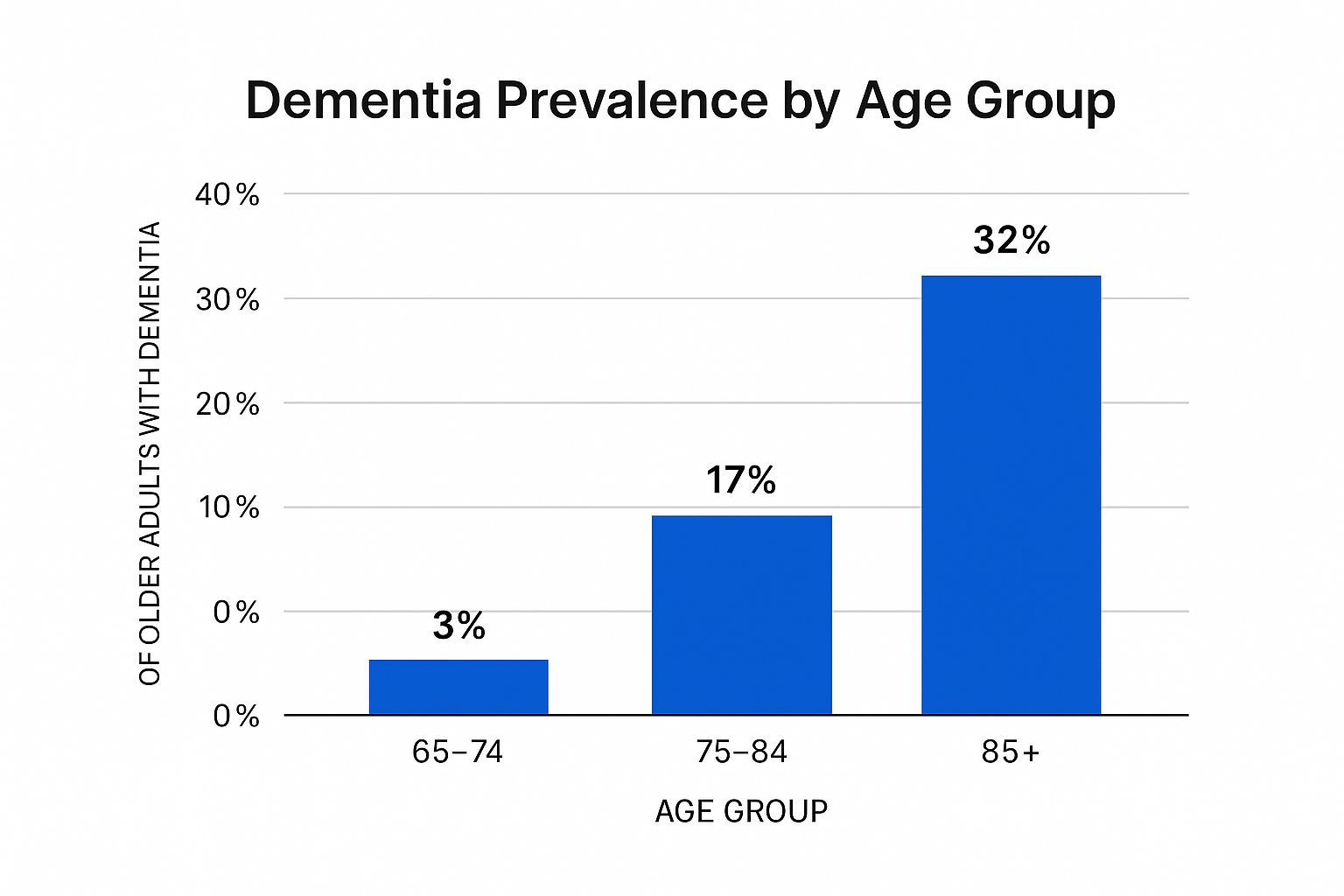
This infographic illustrates how common dementia is across various age groups. The data clearly indicates that the risk of developing dementia rises sharply with age, affecting 32% of individuals 85 and older. This emphasizes the increasing need for effective communication strategies as the world's population continues to age. For more information on this topic and others, explore all our categories.
Effective communication is essential for the well-being of individuals living with dementia. The World Health Organization (WHO) estimates that roughly 57 million people worldwide were living with dementia in 2021, with most residing in low- and middle-income countries. This underscores the importance of developing communication approaches that are both culturally sensitive and accessible. With dementia cases expected to reach 139 million by 2050, adapting our communication techniques will be crucial for supporting this expanding population. Learn more about dementia statistics.
Recognizing Communication Breakdowns
Understanding the specific communication difficulties linked to each stage of dementia can greatly improve how we interact with those affected. In the early stages, you might notice subtle problems with word-finding or following along in conversations. As dementia progresses, these challenges become more obvious, leading to increased confusion, difficulty understanding complex sentences, and a greater reliance on non-verbal cues. In the later stages, communication may primarily depend on facial expressions, gestures, and the tone of voice.
To better illustrate these changes, let's examine a table outlining the impact of dementia on communication abilities throughout its progression.
How Dementia Affects Communication Abilities
| Communication Aspect | Changes in Early Stage | Changes in Middle Stage | Changes in Late Stage |
|---|---|---|---|
| Finding Words (Anomia) | Occasional difficulty recalling specific words. | More frequent word-finding difficulties; may substitute words or use circumlocution. | Significant difficulty finding words; may rely on non-verbal communication. |
| Understanding Language | Difficulty following complex conversations or instructions. | Challenges understanding longer sentences or abstract concepts. | Primarily understands simple phrases and non-verbal cues. |
| Memory | Forgetfulness and difficulty recalling recent events. | Increased forgetfulness; may repeat questions or stories. | Limited short-term memory; primarily relies on long-term memories (which may also be fragmented). |
| Initiating Conversations | May be less likely to start conversations. | Difficulty initiating and sustaining conversations. | Rarely initiates conversations. |
| Non-Verbal Communication | May rely more on gestures and facial expressions to supplement verbal communication. | Increased reliance on non-verbal communication. | Primarily communicates through non-verbal cues such as facial expressions, gestures, and vocalizations. |
This table highlights the progressive decline in communication abilities as dementia advances. Recognizing these changes can help caregivers and family members adapt their communication strategies to better connect with their loved ones. By focusing on simpler language, non-verbal cues, and creating a supportive environment, we can maintain meaningful interactions throughout the different stages of dementia.
Verbal Techniques That Actually Work
Forget what you think you know about conversations. Communicating with someone who has dementia requires a unique approach. Instead of facts and logic, prioritize a comfortable and supportive environment. This change in perspective can significantly improve your interactions.
Simplifying Language and Asking Clear Questions
Asking open-ended questions, such as "What did you do today?" can overwhelm someone with dementia. Instead, ask specific, yes/no questions like, "Did you enjoy your lunch today?" This simplifies the cognitive demands and makes responding easier. Also, avoid complex sentences and excessive pronouns. Keep your language clear, concise, and present-focused.
Validating Feelings and Redirecting Conversations
Resist correcting mistaken beliefs. If someone says, "I need to get home to my mother," avoid responding with, "Your mother passed away years ago." This can be upsetting. Instead, validate their feelings: "It sounds like you're feeling homesick. Tell me about your mother. What was she like?" This acknowledges their emotions and redirects the conversation. Understanding the neurological impact can improve communication. Consider the insights in this article on How Does Addiction Affect The Brain.
The Importance of Patience and Empathy
Patience is essential when communicating with someone experiencing dementia. They might repeat questions or stories. Respond calmly each time. View these repetitions as connection opportunities. An estimated 6% to 10% of people over 65 have dementia, and prevalence increases with age. This highlights the importance of age-sensitive communication. Learn more here. You might also find this resource on senior care helpful. Even small language adjustments can make a big difference.
Creating a Positive Communication Environment
The environment is also crucial for effective communication. Minimize distractions such as loud noises or cluttered spaces. Maintain eye contact and use a gentle, reassuring tone. These adjustments can improve comprehension and reduce anxiety. Combining these verbal techniques with a supportive environment fosters meaningful connections and enhances well-being.

Beyond Words: The Power of Non-Verbal Connection
When communicating with someone living with dementia, words are only part of the equation. Non-verbal communication, including body language, facial expressions, and touch, can often convey more meaning than spoken language. This becomes especially important as dementia progresses and language skills decline. Learning to use non-verbal cues effectively can significantly improve your interactions and strengthen your bond.

The Impact of Body Language and Facial Expressions
Your facial expressions and posture communicate volumes. A warm smile and a relaxed posture project comfort and safety, while a furrowed brow or tense stance can unintentionally cause anxiety. Maintaining eye contact, when culturally appropriate, shows attentiveness and respect. However, avoid prolonged staring, which can feel confrontational.
Subtly mirroring the person's body language, such as reflecting their posture or gestures, can also build connection and understanding. This creates a sense of shared emotional space, making communication and trust easier.
The Role of Touch
Touch is a powerful tool for connection, but it's essential to use it mindfully. A gentle hand on the arm or shoulder can offer reassurance and comfort, particularly during moments of confusion or distress.
However, always be aware of personal space and individual preferences. Some individuals with dementia may be sensitive to touch. Approach with sensitivity and respect their boundaries. Observe their reactions and adapt your approach as needed. This sensitivity is key to building and maintaining trust.
Creating a Supportive Environment
The physical environment significantly impacts non-verbal communication. A calm and organized space can reduce anxiety and promote clearer interaction. Minimize distractions like loud noises or excessive clutter.
Consider the lighting. A brightly lit room can be stimulating, while a dimly lit one can be calming, depending on the individual's preference. Comfortable seating is also essential. Sitting at eye level, rather than standing over someone, fosters a sense of equality and respect. These details contribute to a positive and productive communication experience.
Adapting to Different Stages of Dementia
As dementia progresses, non-verbal communication becomes even more critical. Individuals in later stages might lose the ability to understand words, but they can still perceive and respond to emotions conveyed through facial expressions, tone of voice, and touch.
Maintaining a calm and reassuring presence, even when words are no longer effective, can provide comfort and security. Adjusting your communication strategies as dementia progresses is vital for preserving meaningful interaction.
Navigating Cultural Differences in Dementia Care
Communication can be tricky, and when dementia is involved, cultural nuances add another layer of complexity. How we express ourselves, understand others, and view appropriate support are all shaped by our cultural backgrounds. This means a helpful communication strategy in one culture could be misunderstood or even offensive in another. This section explores how cultural values influence both how dementia is expressed and the effectiveness of different communication approaches.
Understanding Cultural Variations in Dementia Expression
Cultural values significantly affect how individuals experience and express dementia. For example, in some collectivist cultures, families might see cognitive decline as a natural part of aging. They may manage caregiving internally, without outside help. This differs from individualistic cultures where seeking professional help is more common.
Religious beliefs can also influence how families interpret and respond to dementia-related behaviors. Some cultures may attribute memory loss to spiritual factors, while others may view it as a medical condition requiring intervention. Understanding the prevalence of dementia by region is essential for creating effective communication strategies.
In 2020, North America had approximately 5.8 million people living with Alzheimer's and other dementias. Western Europe had about 10 million cases. These regions have different cultural and linguistic nuances that must be considered when developing communication plans.

North America emphasizes personalized care, which involves understanding individual preferences and history to communicate effectively. Western Europe often focuses on community-based care, where communication involves more family and social interaction. Asia, with the highest number of dementia cases, presents unique challenges due to its diverse languages and cultural practices, requiring localized communication approaches. Learn more about dementia statistics.
To further illustrate these regional differences, let's examine the table below:
Regional Approaches to Dementia Communication
This comparison table highlights different communication approaches across major global regions based on cultural values and care systems.
| Region | Cultural Emphasis | Typical Communication Approach | Key Considerations |
|---|---|---|---|
| North America | Individualism, Independence | Personalized care plans, direct communication | Patient autonomy, incorporating personal preferences |
| Western Europe | Community support, family involvement | Collaborative care, family meetings | Family dynamics, social support systems |
| Asia | Filial piety, respect for elders | Indirect communication, nonverbal cues | Cultural sensitivity, language barriers |
This table summarizes some key differences in how communication is adapted to various cultural contexts in dementia care. Note the emphasis on individualized approaches in North America compared to the importance of family and community in other regions.
Adapting Communication Strategies to Individual Backgrounds
When communicating with someone with dementia from a different cultural background, consider their individual history and values. Avoid stereotypes. Instead, learn about their experiences, including their upbringing, language preferences, and social customs. This personalized approach builds respect and trust.
For instance, if someone comes from a culture where direct eye contact is disrespectful, avoiding eye contact can make them feel more comfortable. If touch is considered inappropriate, relying on verbal cues becomes more important. Cultural sensitivity is key, and learning more about emotional intelligence can be beneficial.
Addressing Generational and Historical Influences
Generational experiences, like living through war or significant social change, also affect communication. Individuals who experienced trauma might be more sensitive to certain topics or communication styles. For example, raising your voice, even unintentionally, could trigger anxiety in someone who experienced war-related trauma.
Understanding these sensitivities allows you to tailor your communication, fostering a safer and more supportive interaction. By acknowledging and respecting these generational and historical influences, you can improve communication and strengthen connections with individuals living with dementia.
Handling Difficult Moments With Compassion
Even with the best communication strategies, difficult situations are bound to happen when interacting with someone who has dementia. These can range from aggressive behavior to instances of non-recognition. This section offers practical advice for navigating these sensitive moments with compassion and empathy. Learning how to de-escalate stressful situations, redirect challenging conversations, and validate feelings will be essential.
Addressing Accusations and Suspicions
Individuals with dementia sometimes become suspicious or accusatory. They might misplace belongings and think they've been stolen, or misunderstand your actions. Responding with logic often doesn't help. Instead, try empathizing and offering reassurance. Instead of arguing, try saying, "I understand how frustrating it is to lose something important. Let's look for it together."
Responding to Questions About Deceased Relatives
One of the most challenging scenarios occurs when a loved one asks about someone who has passed away. Reminding them of the death can cause renewed grief. Instead of correcting them, acknowledge their feelings. If they ask for their mother, try responding with, "You miss your mother. What are some of your favorite memories of her?" This approach allows you to engage positively without contradicting their perception.
Navigating False Memories and Delusions
People with dementia can sometimes develop false memories or experience delusions. Instead of disagreeing with them, try briefly entering their world. Validate their feelings and then gently redirect the conversation. For instance, if they believe they are late for work, you might say, "It sounds like you have a busy day planned. What did you enjoy most about your job?" This acknowledges their feelings before gently shifting to a calmer topic.
Managing Agitation and Aggression
Agitation or aggression can arise for various reasons, such as pain, discomfort, or overstimulation. Try to identify the root cause. Ensure the individual is comfortable, not in pain, and not overstimulated. Speak in a calm, soothing voice and avoid sudden movements. If the behavior escalates, prioritize your safety and consider contacting a healthcare professional.
Remembering the Person Behind the Dementia
During challenging moments, it's easy to feel frustrated. It's important to remember that the person with dementia isn't purposely being difficult. Their behavior is a result of the disease. Taking deep breaths, practicing patience, and focusing on connecting with the individual can help you manage difficult situations with compassion. How you communicate with someone who has dementia greatly impacts both their well-being and your own.
Tech Tools That Transform Communication
Technology offers a wealth of tools to improve communication with individuals living with dementia. From simple visual aids to sophisticated apps, these tools can help bridge communication gaps and strengthen connections. However, it’s crucial to choose the right technology based on individual needs and abilities. This includes considering the person's stage of dementia, comfort level with technology, and sensory preferences.
Low-Tech Tools for Enhanced Communication
Sometimes, the simplest solutions are the most effective. Visual aids, such as picture cards of common activities or objects, can be incredibly helpful. These cards can assist individuals in expressing their needs and wants, particularly as verbal communication becomes more difficult. Similarly, memory books with photos and labels can encourage conversation and reminiscence. Even a simple whiteboard with daily schedules or reminders can provide structure and reduce anxiety.
Exploring Specialized Apps and Software
Several apps are designed specifically for communicating with people who have dementia. Some apps offer simplified interfaces for video calls, allowing easier connection with family and friends. Others provide memory games and cognitive stimulation activities to help maintain mental acuity. When introducing new technologies, start slowly and offer ample support. You might be interested in: How to Master Job Listings.
The Role of Digital Picture Frames and Sensory Tools
Digital picture frames filled with family photos can spark conversations and bring back cherished memories. These can be particularly beneficial for individuals in the later stages of dementia who may have difficulty recognizing loved ones. Sensory tools, such as weighted blankets or fidget toys, can offer comfort and reduce agitation, fostering a more positive environment for communication.
Considering AI Companions and Voice Assistants
While still a developing area, AI companions and voice assistants like Alexa show potential for assisting individuals with dementia. These tools can offer reminders, play music, and even engage in simple conversations. However, it’s important to consider the ethical implications of using AI in dementia care and ensure responsible use of the technology.
Practical Implementation and Cost Considerations
When selecting tech tools, consider the cost and ease of use. Some apps and software require subscriptions, while others are free or involve one-time purchases. Simple tools like picture cards and whiteboards are typically inexpensive and easy to implement. It’s also important to assess the effectiveness of each tool over time and adapt your approach as needed. Introducing new technologies gradually and providing ongoing support, like demonstrating how to use the tool and ensuring easy access, can maximize their benefit. Remember, technology should enhance, not replace, human interaction. While these tools can be valuable, the strongest connection stems from genuine human connection, patience, and understanding.
For compassionate and personalized in-home care for your loved ones in Princeton, NJ, and the surrounding Mercer County area, contact Caring Hands Senior Services at https://caringhandsseniorservices.org. We offer a range of services designed to meet the unique needs of individuals with dementia, including personal care, nursing services, respite care, and companionship.


